Surviving A Deadly Heart Attack
With cardiovascular disease (CVD) being the leading cause of mortality and morbidity among the western population, it is not a long shot for one to think almost everyone knows someone that has encountered heart disease or the symptoms thereof. Not surprising that I had the opportunity to meet these people whom I am now writing.

There was a cardiologist at a well-known and respected institution that suggested, her patient, a 60 year old man with two occluded arteries and only a functioning aorta (widow maker) had on average 10 years to live. The patient had one silent heart attack and one where he sought medical treatment. During that time the cardiologist attempted to place a stent to reopen the artery, but had no success due to the “amount of scarring.” Which is why the patient was left with two arteries occluded. I am left to wonder, with all the research that is being conducted to extend life and improve cardiac health including but not limited to pharmaceuticals and the surgical techniques, why is there nothing that can be done other than sending this patient home with a bleak outlook on the next several years of his life. That patient is still alive and doing well, thanks for asking. That is not an isolated case of patients being sent home hopeless. I came across a story on Facebook (2014) about a 58 year old lady that was on hospice for the last four years. She presented to the hospital in full cardiac arrest. The emergency medical team was performing compressions until she arrived at the hospital; thankfully they were able to revive her. She previously suffered 3 heart attacks resulting in 2 triple bypass surgeries, but after that 4rd heart attack in August 2010 the doctors said there was nothing they could do to improve her [cardiac] health. Before you are alarmed, she had multiple chronic illnesses by this time: 3 myocardial infarction (MI), congestive heart failure, diabetes, breast cancer (resulting in double mastectomy), hypertension, and renal failure. Since she was not a good candidate for dialysis, she had a poor prognosis. She was taken off all her medications (from a cocktail of 19 pills to 4, which were for CVD symptoms and a morphine tablet for pain) and the end of life care team made worked diligently to make her comfortable until she passed. The medical providers alerted the family that she could pass on at any time. That was in 2010, it is now 2018 and she is STILL alive and well! Both patients are. So, what allowed this Facebooker to live so long with no major arteries? How is this even possible? Is it a case of faith/a miracle alone (which is what the Facebook post suggest) or something that can be medically/scientifically explained? What about the man from the former story? Is 10 years the best he could hope for or is the case with the latter possible in his case? Is there anything we can do pharmaceutically to drive the system toward the former?
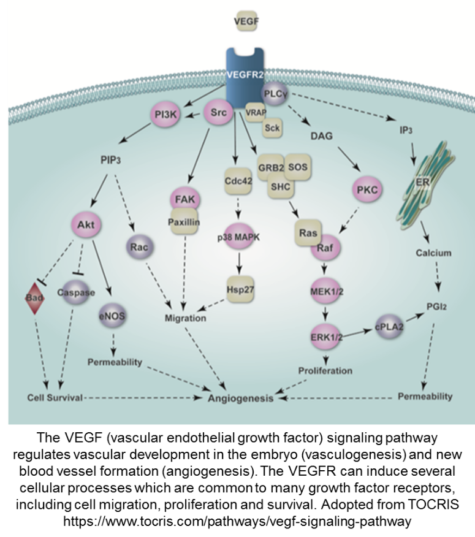
In a 2018 study by Manavski et al, it was suggested that angiogenesis after ischemia is due to clonal expansion of endothelial cells. Indicating there is, indeed, a scientific rationale for the revascularization of the aforementioned hearts. After an MI there is significant scar tissue leading to the inability for the heart to provide the necessary oxygen and nutrients to other organ systems, known as ischemia. The newly ischemic environment potentiates the growth of new vessels to compensate for the loss of cardiac output due to the MI. These vessels are said to be generated through a mechanism known as angiogenic sprouting; in excess this pathological growth that can promote tumor formation. The signaling molecule vascular endothelial growth factor (VEGF) is hallmark in the formation of new vessels, but it is also highly expressed in cancers. Before we get off track, let’s think about the mechanisms in play in an MI. monocytes are attracted to an insult in the vessel, they differentiate into macrophages, those macrophages take up oxidized low density lipoproteins, and since they cannot process them, they die (undergo apoptosis). In ischemia macrophages promote the development of collateral vessels, but in tumors macrophages (M2) produce proangiogenic factors while educating the macrophage as what phenotype to take on – Tumor or cardiac. There are signals in the body that include VEGF and Ang1 that keep endothelial cells inactive to promote vessel stabilization. Furthermore, an oxygen sensor helps the endothelial cells to normalize and readapt to oxygen supply to the organ tissues. There are a battery of enzymes that play a role in vessel maturation which is too exhaustive for this blog, but mainly sprouting is impaired by inhibition of VEGF and S1P receptor signaling is the stabilizer for the vasculature.
In conclusion, having a heart attack is not necessarily a death sentence. Even when all the arteries to the heart of occluded. It is not the norm, but the human body is an overwhelmingly amazing in compensating for the loss of some pathways. Our bodies have system in place with mechanism to support life even when the answers evade medicine and science. With the passion to conduct research, we are finding ways to make our heart health better daily. As we explore mechanistic pathways to reduce oxidative stress, inflammation, and other underlying pathways, it is up to each individual to maintain a healthy heart by following the guidelines set in place by the American Heart Association. As for the patients above, they are working with their medical teams to maintain a healthy life. May I suggest you all continue to seek your physicians’ advice on how to improve/maintain your heart health?

Anberitha Matthews, PhD is a Postdoctoral Fellow at the University of Tennessee Health Science Center in Memphis TN. She is living a dream by researching vascular injury as it pertains to oxidative stress, volunteers with the Mississippi State University Alumni Association, serves as Chapter President and does consulting work with regard to scientific editing.