For this month’s blog entry, I’ve decided to share a more reflective piece. In now just over six months into my young career, my early morning routine is pretty set in stone. Wake up. Shower. Scrubs. Coffee. Mask. Keys. Go! But what happens from approximately 8 am – 5 pm is still evolving.
This blog will briefly go over my daily struggles, but I could just as easily share five daily rewards/positives/joys of an early career physician … and maybe next month I will.
- I’m the attending (physician). Part of being fresh out of training is that nobody knows. Whether you stay at your home institution or move to a new setting, you’re likely the new kid on the block in the Doctors’ Lounge or the EMR’s attestation text box. Despite proudly wearing my “attending physician” ID badge, I find myself constantly having to reiterate that I’m the supervising doctor. I recently entered the room to begin time out for a transesophageal echo and was stopped by the anesthesiologist because we couldn’t begin the case without the cardiologist present. Another time, I was asked if I was the fellow doing the case with Dr. X, a well-known echocardiographer. Despite how this may sound, I quite like the shocked look on my patient’s faces when I walk in and introduce myself as the person who will be managing their complex cardiovascular disease – or my ability to walk through the medical center unbothered and largely unnoticed while taking in some much needed Miami sun.
- One of my daily struggles is not knowing how to say “no.” As a medical trainee, you’re often the person called upon to do the tasks that no one else wants to take on. Whether it be consent for a procedure or calling the pharmacy to correct a prescription, you’re often faced with the rhetorical question of “can you please…?” or “ would you mind…?” Well, this doesn’t really stop when you’re a newly appointed faculty. I often reply to emails first or make phone calls because I’ve been there and I know that I CAN help in that way. Eventually, though, I will need to learn when this is impinging on time that could be well allocated to more important tasks.
- To do or not to do. From the moment my first patient shares with me the reason for their visit, there is a tug-o-war in my head between doing something and doing nothing. A wise professor once told me that 70% of medical conditions resolve without the doctor doing anything. We’re tasked with identifying the 30% of the time when we can make an impactful difference in the disease course. I once read a Wall Street Journal article titled “When Doing Nothing is the Best Medicine.” This is much easier said than done, but I’ve found that many patients just want reassurance that what ails them will not lead to their untimely demise. Explaining my thought process, and clearly stating that we can always order more tests or perform more studies at a later date if things don’t get better, has served me well so far.
- Leaving work at work. It’s not uncommon to find a trainee spending extra time in the hospital or in the clinic finishing tasks that their attending doesn’t want to find undone in the morning. When you’re the attending, the decision as to what can wait until later lies with you. When I first started my new job, I often stayed up late replying to emails or finishing notes, or making calls from home. What I’ve found is that not everything needs to be done now. I have frequently reminded myself of the following diagram, as it has helped me leave work at work and not take it home with me.
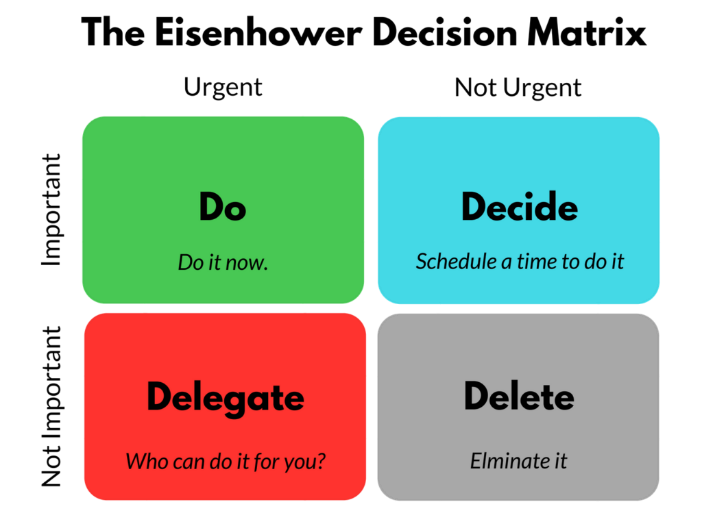
Source: https://luxafor.com/the-eisenhower-matrix/
- Work/Life Balance. As physicians, we’re tuned to work work work until you can’t work anymore. It’s commonplace for physicians to work well past the retirement age, and sometimes until they are no longer with us. My mentors have shared with me that the decision to prioritize family, vacation, rest starts NOW. It is a lot harder to put into practice. There is always something that needs to be attended to, whether your “out of work” auto-reply is posted or not. I’ve made it a goal of mine to fully utilize the ample paid time off afforded to me by my employer, and to truly disconnect during these times. It’s still very hard, and I haven’t perfected it, but making it a priority is the first step.
Thank you for reading, and please share with me some struggles that you’re having as an early career physician. I can be reached on Twitter @DrDapo. Until next time!
“The views, opinions and positions expressed within this blog are those of the author(s) alone and do not represent those of the American Heart Association. The accuracy, completeness and validity of any statements made within this article are not guaranteed. We accept no liability for any errors, omissions or representations. The copyright of this content belongs to the author and any liability with regards to infringement of intellectual property rights remains with them. The Early Career Voice blog is not intended to provide medical advice or treatment. Only your healthcare provider can provide that. The American Heart Association recommends that you consult your healthcare provider regarding your personal health matters. If you think you are having a heart attack, stroke or another emergency, please call 911 immediately.”