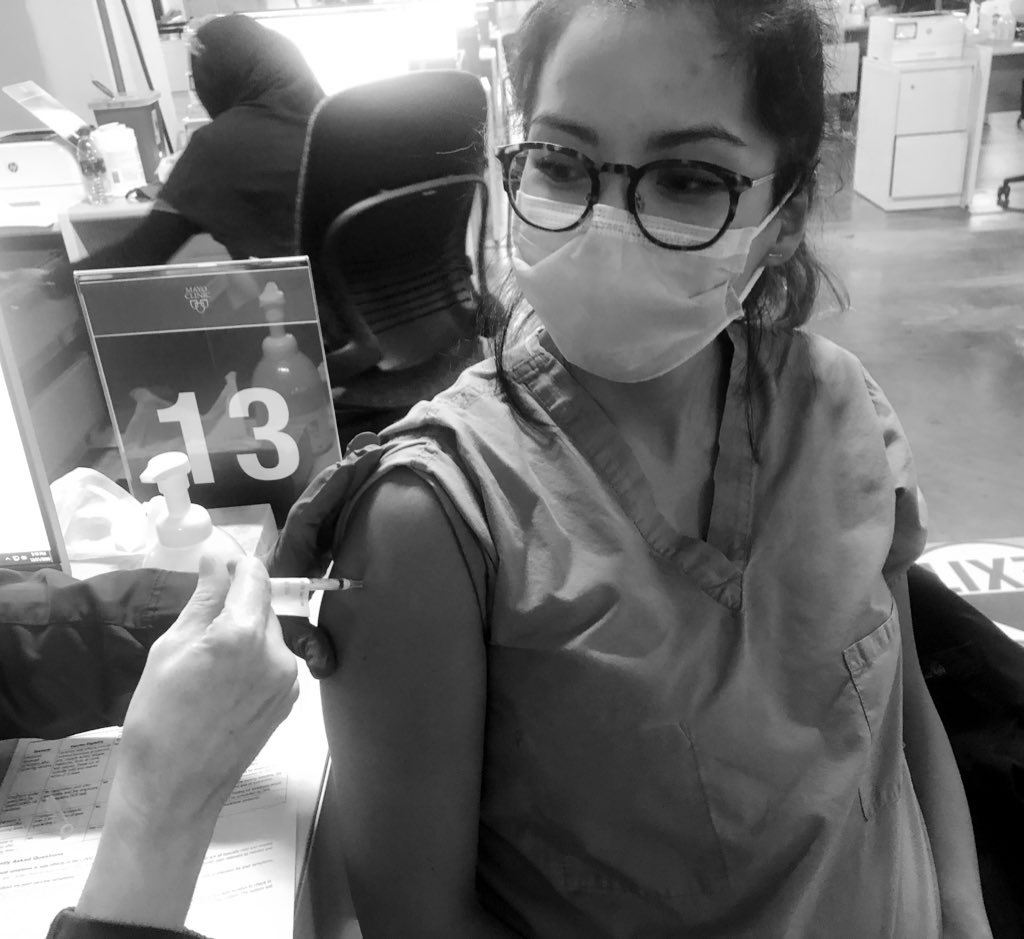
 When news of the approval of the Pfizer vaccine surfaced, I felt a sense of anxiety. There was no data on pregnant women in the COVID-19 vaccine trials. As a medical professional, we have been trained to apply for evidenced-based medicine and baseline patient characteristics of trial participants to the patients we plan to treat. But what if your pregnancy status was not studied in the trial during a global pandemic? How might you weigh the unknown risks of the vaccine to your growing fetus with the risk of COVID-19 infection while pregnant?
When news of the approval of the Pfizer vaccine surfaced, I felt a sense of anxiety. There was no data on pregnant women in the COVID-19 vaccine trials. As a medical professional, we have been trained to apply for evidenced-based medicine and baseline patient characteristics of trial participants to the patients we plan to treat. But what if your pregnancy status was not studied in the trial during a global pandemic? How might you weigh the unknown risks of the vaccine to your growing fetus with the risk of COVID-19 infection while pregnant?
Making the Decision
A few days passed when I received an email from Occupational Health that my cardiology fellowship program would be part of the Phase I distribution of the vaccine. The following day, my midwife conveyed to me that the OB department would align with the American College of Obstetrics and Gynecology (ACOG) Practice Advisory Statement:
“ACOG recommends that COVID-19 vaccines should not be withheld from pregnant individuals who meet criteria for vaccination based on ACIP-recommended priority groups.”
I felt a sense of relief that I would not be prohibited from getting the vaccine if I chose to do so yet also felt a sense of panic when I read the following:
“Vaccines currently available under Emergency Use Authorization (EUA) have not been tested in pregnant women. Therefore, there are no safety data specific to use in pregnancy.”
As a trained medical professional and protective mother, the overwhelming number of daily decisions we make to ensure the safety of our babies are overwhelming- no sushi, no wine, no retinoids or other harmful active ingredients found in our beloved skin care regimens, no hot tubs… I could go on.
However, the challenge of navigating the emotions of fear and uncertainty about the vaccine became incomparable to the following facts:
mRNA Does Not Alter Your DNA
These vaccines are not live virus vaccines and do not use an adjuvant to augment the efficacy of the vaccine. It does not enter the nucleus or alter human DNA.
Risk of Exposure
My job involves routinely interacting with patients and performing aerosolizing procedures, which places me at increased risk for exposure to COVID-19.
Symptomatic Pregnant Patients Infected With COVID-19 Are at Increased Risk of Severe Illness
This includes hospitalization in the intensive care unit (ICU), the need for intubation and mechanical ventilation, extracorporeal membrane oxygenation (ECMO), and death.
I decided that getting vaccinated was safer than getting COVID-19. I also consulted with my partner who is also my husband and the father to our developing fetus. Although ultimately it was my decision to make, I felt comforted knowing he was 100% on board with me proceeding with vaccination based on the above as well.
Getting Vaccinated and the Side Effects
I received both doses of the Pfizer vaccine, the first dose at 20 weeks and the second dose at 23 weeks gestation. With the first dose of the vaccine, I only experienced arm soreness that peaked on day two. With the second dose, I experienced a mild headache and mild bilateral upper extremity soreness but with two doses of acetaminophen, I continued to work at full capacity and performed intraoperative transesophageal echocardiograms without issues.
I am now 25 weeks pregnant and feel a sense of pride that I made this decision to protect myself and my unborn child. I have received many texts and messages inquiring about how I made my choice. Questions such as “would your decision change if you were in your first trimester before organogenesis was complete?” or “would you get vaccinated while trying to conceive?” were a few memorable ones. I firmly believe it is your right as a woman to make this difficult decision when there is no safety data available. Personally, yes, I would have still made the decision to vaccinate.
Lastly, I will join many of the other scientists and advocates out there who demand that pregnant and lactating women be included in future vaccine research trials http://vax.pregnancyethics.org/prevent-guidance. Track records of vaccine safety should exist for expectant mothers to help guide and improve vaccination rates. Here is to hoping for a better year that allows each and every one of us access to the COVID-19 vaccine no matter what country, gender, pregnancy status, lact
ation, status, or employment status we bear.
Stay safe and stay healthy,
Kyla Lara-Breitinger, MD, MS
References:
https://www.acog.org/clinical/clinical-guidance/practice-advisory/articles/2020/12/vaccinating-pregnant-and-lactating-patients-against-covid-19
https://s3.amazonaws.com/cdn.smfm.org/media/2632/FDA_final.pdf
“The views, opinions and positions expressed within this blog are those of the author(s) alone and do not represent those of the American Heart Association. The accuracy, completeness and validity of any statements made within this article are not guaranteed. We accept no liability for any errors, omissions or representations. The copyright of this content belongs to the author and any liability with regards to infringement of intellectual property rights remains with them. The Early Career Voice blog is not intended to provide medical advice or treatment. Only your healthcare provider can provide that. The American Heart Association recommends that you consult your healthcare provider regarding your personal health matters. If you think you are having a heart attack, stroke or another emergency, please call 911 immediately.”