In medicine, there is no widespread list of medical programs that are considered inclusive. During this time, the cardiology community has both publicized the need for addressing racial bias in medicine and advocating for inclusivity. Dr. Quinn Capers IV, who is an interventional cardiologist and appointed the Chair of the ACC’s Diversity and Inclusion Committee in 2020, has made great strides in this effort. Dr. Capers has traveled the country describing the experience of BIPOC (Black Indigenous People of Color) patients and physicians. He is presenting to different institutions to tackle racial bias in medicine. Drs. Laxmi Mehta, Sharonne Hayes, Toniya Singh, and additional exceptional colleagues have identified concerning data regarding discrimination, harassment, and a hostile work environment (HWE) in cardiology. They found higher rates of HWE in women (68%, over three-fold higher than men) and African Americans (53% with 46% increased odds compared to Whites). These issues require real solutions and likely have deep roots for BIPOC (‘Equity & Inclusion in Medicine Part II’). The importance of including more BIPOC in medicine is to increase community representation. The less community representation we have, the more progressive community chronic disease and inequity we will see.
As programs grow to understand how to boost the numbers of underrepresented minorities in general, it is also important for trainees to know which programs are considered supportive currently. Therefore, I decided to identify which specific programs were considered inclusive. Further, the goal of this inquiry was to share the names of these programs to the cardiology community interested in boosting diversity and inclusion (D&I).
In October of 2020, I sent out a Facebook posting to a group of African American physicians and dentists. I polled the group to ask which medicine programs were inclusive. All members were included to answer with no one excluded. A tally was created each time a member mentioned a program with the addition of ‘likes’.
After a follow-up time of approximately a week, there were 97 mentions and 329 tallies with the addition of ‘likes’. A total of 15 (4.5%) was the highest tally. The top three programs and specialties on the list were Emory – Emergency Medicine, Johns Hopkins-Internal Medicine, University of Chicago- Emergency Medicine (15,14,13 tallies respectively). The programs with the most frequent mentions were Baylor, Emory, and Mayo Clinic (mostly Minnesota) (5 mentions each). The most frequent specialties mentioned were family medicine (15), emergency medicine (11), internal medicine (11), and OB-GYN (11). In terms of cardiology, the top-rated programs in this specialty were Duke, Mayo Clinic, and Marshall with one tally each. I did a separate poll from a group of BIPOC/African cardiology fellows and the top program mentioned as being diverse and inclusive more than once was Duke. Other programs mentioned were Yale, Vanderbilt, SUNY Downstate, Mayo Clinic Arizona and Florida, UPENN, Rush, and the University of Kentucky Lexington. What constituted inclusive for the cardiology group came down mostly to pure numbers.
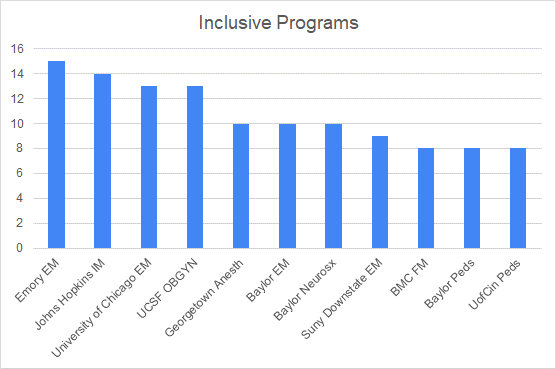
*EM-emergency medicine, *IM-internal medicine, *Anesth-anesthesia, *Neurosx-neurosurgery, *Peds-pediatrics, *FM-family medicine
This list is a helpful initial guide based on physician feedback regarding program diversity and inclusivity. This is a relatively novel approach to receiving feedback regarding D&I with crowdsourcing from social media/WhatsApp. Certainly, not all programs were represented, so one cannot extrapolate negative inclusivity from the lack of mention. As well, there may be a selection bias towards a program or specialty related to the group composition. Further, for both groups, this poll was on social media/WhatsApp and they may not have been alerted to it with busy training schedules.
Cardiology is a specialty that is encouraging diverse recruitment and aiming to create an environment of appreciation for fostering inclusivity (see ‘Equity & Inclusion in Medicine Part III’). The top programs have clearly invested time and resources into recruitment and retention. Cardiology program directors may benefit from their strategies. The goal of improving the number of underrepresented trainees in cardiology could boost curriculum innovation, incorporate a broader reach to a diverse patient population, and improve mentorship for URIM medical students and residents.
“The views, opinions and positions expressed within this blog are those of the author(s) alone and do not represent those of the American Heart Association. The accuracy, completeness and validity of any statements made within this article are not guaranteed. We accept no liability for any errors, omissions or representations. The copyright of this content belongs to the author and any liability with regards to infringement of intellectual property rights remains with them. The Early Career Voice blog is not intended to provide medical advice or treatment. Only your healthcare provider can provide that. The American Heart Association recommends that you consult your healthcare provider regarding your personal health matters. If you think you are having a heart attack, stroke or another emergency, please call 911 immediately.”