Elevated cholesterol levels or hypercholesterolemia can be found for years or even decades, before individuals present with cardiovascular disease and complications such as myocardial infarction, stroke, or sudden cardiac death. The diagnosis of hypercholesterolemia and its treatment along with healthy lifestyle changes including a healthy diet and exercise as well as blood pressure control, are cornerstones of long-term cardiovascular health.1
There has been a substantial decline in cardiovascular disease mortality in the last decade due to improved awareness, therapy for established cardiovascular disease and primary and secondary preventive interventions.1 However, this observation is absent in young adults.2 Over the last decade, unfavorable trends in coronary heart disease and related mortality in younger individuals, i.e. 35-55 year-old, have emerged.2
We have previously shown that there is a phenotype of young adults with premature hypertension and development of resistant hypertension in their 30s.3 This phenotype has been characterized in a cross-sectional study of 2068 patients seen in a university referral clinic for resistant hypertension. In this study 45% of consecutively seen patients were younger than 55 years of age. Amongst them, 23% had high lipids, 25% were obese, 19% had diabetes, and 13% had obstructive sleep apnea. Cardiovascular events such a s history of myocardial infarction, stroke, or heart failure were prevalent were found in >20%. The majority of these predominately obese, resistant hypertensive individuals have excessive aldosterone, cortisol and sodium levels, conditions that are associated with increased cardiovascular morbidity and mortality, independent of blood pressure levels.
Lipid-lowering drugs, so-called statins, have been shown to reduce cardiovascular disease and mortality. Lipid lowering with statins in patients with hypercholesterolemia has a proven survival benefit for both primary prevention (ie, in patients without clinical evidence of coronary disease) and secondary prevention (ie, in patients with established coronary disease), even when serum cholesterol concentrations are “normal” for the population or borderline high. The mechanisms by which lipid-lowering therapy is beneficial are incompletely understood since absolute levels of cholesterol before or during treatment only explain parts while cholesterol-independent effects have been also described.1 Among the non-lipid mechanisms that may be involved are plaque stabilization, reduced inflammation, improvement of endothelial and arterial function, and decreased blood clotting.
In 2013 the American College of Cardiology and American Heart Association developed a new guideline for the management of hyperlipidemia. While previous guidelines recommended to initiate or adjust predominantly in response to lipid values these 2013 ACC/AHA guidelines target patients to fixed dose of statin therapy corresponding to atherosclerotic cardiovascular disease (ASCVD) or other risk factors. The four at-risk populations of individuals that are thought to benefit from statin therapy based on this guideline include:
- Adult patients with clinical ASCV
- Adult patients with primary elevations of LDL–C ≥190 mg/dL
- Patients 40-75 years of age with diabetes and LDL–C 70 to 189 mg/dL without clinical ASCVD
- Patients 40-75 years of age without clinical ASCVD or diabetes with LDL–C 70 to 189 mg/dL and have an estimated 10-year ASCVD risk of 7.5% or higher
In our cohort half of obese young patients under the age of 40 would per se not qualify to be treated with a statin. Patients between the ages of 40-55 are in the majority of cases not considered “eligible” since age is one of the most powerful nominators in the risk calculator and, anecdotally, when we evaluate these patients for statin eligibility for primary prevention, we usually calculate an estimated 10-year CVD risk score of <5%.
At their first visits we always discuss life style changes, since younger patients may be more motivated to eat healthier, exercise, and lose weight, but consistent, successful lifestyle changes are often difficult to accomplish.
When we consider statin treatment for primary prevention even if the ASCVD risk score is <7.5%, there are a lot of unknowns. Aside from statins being contraindicated in young women who are or want to become pregnant or are breastfeeding, it is not known if there are short-term benefits of therapy. There are few data on the safety of statins over decades of therapy and possible side effects of statin therapy could outweigh potential benefits.
Furthermore, we don’t know whether long-term treatment leads to better outcomes and who are the individuals who are going to benefit. With evolving advances in precision medicine, we may be able to “customize” primary prevention especially for this group and identify young individuals in whom premature cardiovascular events can be prevented.
However, the question remains: how can we prevent cardiovascular events in young adults?
Data of young adults who suffered a cardiovascular event will help to elucidate underlying mechanisms and optimal therapy regimens.
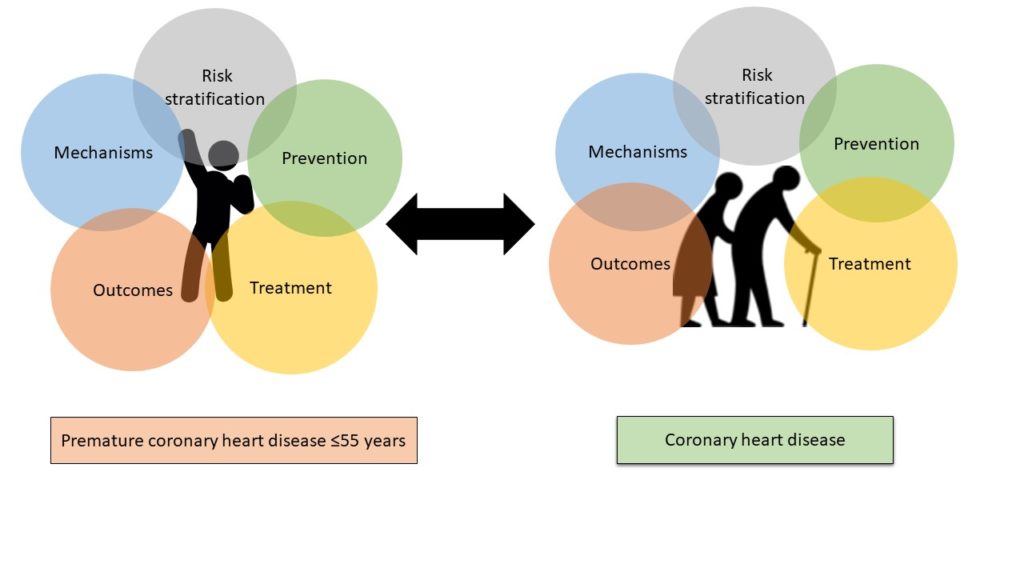
This problem has been recognized and resulted in the YOUNG-MI Registry, a retrospective study examining a cohort of young adults age ≤50 years with a first-time MI. The study uses electronic health records of 2 large academic centers, as well as detailed chart review of all patients, to generate high-quality longitudinal data regarding the clinical characteristics, management, and outcomes of patients who experience a myocardial infarction at a young age. Findings are thought to provide important insights regarding prevention, risk stratification, treatment, and outcomes of cardiovascular disease in this understudied population, as well as identify disparities which, if addressed, can lead to further improvement in patient outcomes.
In a recent study from this registry, Singh et al. analyzed retrospectively the statin eligibility of young adults after a myocardial infarction. In this study the statin eligibility, based on the 2013 ACC/AHA guidelines and 2016 USPSTF recommendations, for primary prevention in adults <50 years who experienced a first-time type 1 myocardial infarction were evaluated. The median age of analyzed patients was 45 years, 20% were women, the majority had at least 1 traditional cardiovascular risk factor and 57% had experienced a ST-segment elevation myocardial infarction. Surprisingly, the median estimated 10-year atherosclerotic cardiovascular disease risk score was only 4.8% (interquartile range 2.8-8.0%). Only 49% and 29% would have met criteria for statin eligibility as per the 2013 ACC/AHA guidelines and 2016 USPSTF recommendations, respectively. These findings were even more noticeable in women where 63% were not eligible for statins according to either one of the guidelines as opposed to 46% of men only. To summarize these findings, the majority of young adults who present with a heart attack would not have met current guideline-based treatment thresholds for statin therapy prior to their myocardial infarction.
It highlights the need for better risk assessment tools for young adults. Further, much more needs to be known about risk profiles, optimal prevention, and treatment to improve outcomes in these young understudied adults.
References
- Stone NJ, Robinson JG, Lichtenstein AH, Bairey Merz CN, Blum CB, Eckel RH, Goldberg AC, Gordon D, Levy D, Lloyd-Jones DM, McBride P, Schwartz JS, Shero ST, Smith SC, Jr., Watson K, Wilson PW, Eddleman KM, Jarrett NM, LaBresh K, Nevo L, Wnek J, Anderson JL, Halperin JL, Albert NM, Bozkurt B, Brindis RG, Curtis LH, DeMets D, Hochman JS, Kovacs RJ, Ohman EM, Pressler SJ, Sellke FW, Shen WK, Smith SC, Jr., Tomaselli GF and American College of Cardiology/American Heart Association Task Force on Practice G. 2013 ACC/AHA guideline on the treatment of blood cholesterol to reduce atherosclerotic cardiovascular risk in adults: a report of the American College of Cardiology/American Heart Association Task Force on Practice Guidelines. Circulation. 2014;129:S1-45.
- Ghazi L, Oparil S, Calhoun DA, Lin CP and Dudenbostel T. Distinctive Risk Factors and Phenotype of Younger Patients With Resistant Hypertension: Age Is Relevant. Hypertension. 2017;69:827-835.
- Ghazi L, Dudenbostel T, Xing D, Ejem D, Turner-Henson A, Joiner CI, Affuso O, Azuero A, Oparil S, Calhoun DA, Rice M and Hage FG. Assessment of vascular function in low socioeconomic status preschool children: a pilot study. J Am Soc Hypertens. 2016.

Tanja Dudenbostel is an Internist, Hypertension Specialist within Cardiology at the University of Alabama at Birmingham where I divide my time as an Assistant Professor between clinical research and seeing patients in cardiology.