Nearly 2 weeks after AHA Scientific Sessions 2017, I’m back at home, sipping coffee on a chilly Sunday morning and thinking about Anaheim. The larger-than-life convention center, the numerous and packed sessions, and the built-in-a-day pharma fueled exhibit halls.
Working backwards, I remember fitting in a lunch sponsored by Amgen, given by Dr. Alan Brown, Director of Cardiology at Advocate Lutheran General Hospital. It boasted boxed lunches but lacked elbow room, but by the end of the hour, I was impressed.
As a trained dietitian, I’m aware of at least some of the challenges in providing patient care. With new lipid guidelines, new blood pressure guidelines, new everything guidelines, up until now, the ease of popping a pill has seemed to rise above the effectiveness of lifestyle changes.
For the first time, I heard physicians calling on one another to sit face-to-face and eye-to-eye with their patients, and ask them about their physical activity. And their eating habits. In Dr. Brown’s words, by asking about these topics, you communicate to your patients that they are important.

(The DASH Diet stands for Dietary Approaches to Stop Hypertension and is rich in fruit, vegetables, low-fat dairy while reduced in saturated fat and cholesterol. Content Provider: CDC/Amanda Mills. 2011)
At this same conference, Dr. Stephen Juraschek presented his results using the DASH diet – “The Effects of Sodium Reduction and the DASH Diet in Relation to Baseline Blood Pressure,” published just a few weeks ago. The investigators randomized adults with pre- or stage 1 hypertension (and not using blood pressure lowering medications) to DASH diet or control diet. Then in random order, over 4 weeks with 5-day breaks, participants were fed at 3 sodium levels: 50, 100, 150 mmol/day at 2,100 kcal. And what did they find? Adopting the DASH diet in combination with reduced sodium intake achieved “progressively greater reductions at higher levels of baseline SBP [≥150 mmHg]”.
So why am I talking about lifestyle modifications in a post about incorporating conference learnings back into your everyday reality at work? Well, a big announcement that came out of AHA17 was the new hypertension guidelines. I noticed recurrent statements and questions about these guidelines, in presentations, on social media, and from my peers when I returned home.
At our first peer led research meeting back from AHA17, I printed off a few copies of the Top Ten Things To Know (PDF) about the 2017 hypertension guidelines. We touched on the implications of new classification categories – more treatment, higher prevalence, changes in comparisons over time in our epidemiologic studies.
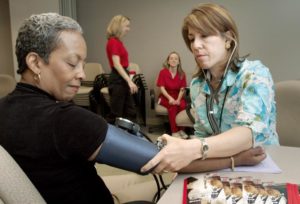
(Connie Alfred (left), of the National Center for Infectious Diseases (NCID), was shown having her blood pressure taken by Robyn Morgan, of the National Center for Chronic Disease Prevention and Health Promotion (NCCDPHP), during a free blood pressure screening event that was held on all CDC campuses in 2005. Content Provider: CDC/CDC Connects. 2005.)
We were happy to see the focus on accurate measurement of BP, ensuring adequate rest time and taking averages of measurements, a technique we use in epidemiologic studies to minimize measurement error. Those of us particularly interested in physical activity and nutrition epidemiology rejoiced at the lifestyle modification efforts. We closed the discussion with an acknowledgement of conflicting and numerous other guidelines, the reality of putting them into practice – from primary care to cardiology clinics – as well as misinformation in the media coverage of the guidelines, such as misquoting the relaxed recommendations for older adults.
With so much to chew on, I closed the discussion encouraging everyone around the table to think more on the implications of new guidelines, and our role in developing them, implementing them, and evaluating them.

Bailey DeBarmore is a cardiovascular epidemiology PhD student at the University of North Carolina at Chapel Hill. Her research focuses on diabetes, stroke, and heart failure. She tweets @BaileyDeBarmore and blogs at baileydebarmore.com. Find her on LinkedIn and Facebook.